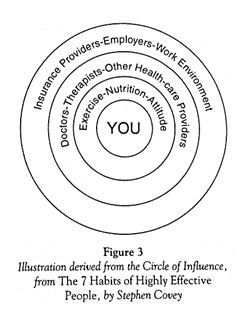
From Chapter 2 of The Pain-Free Program: A Proven Method to Relieve Back, Neck, Shoulder and Joint Pain
First, let’s begin with your doctor. Your doctor is there for you. He or she is not you. In other words, no doctor knows your body better than you do. When you go to the doctor with a complaint about your body, your doctor examines you, runs tests if necessary and then applies a diagnosis to your problem. This diagnosis is based on what the doctor sees, feels with his hands and sometimes hears. Your doctor may also come to a conclusion based on the answers you provide him to targeted questions. But your doctor can never experience what you experience. The pain, the limitations, the inconveniences are all unique to you. There may be similarities to others with a like condition, but never will their experiences be identical to yours. Therefore, this well-educated, well meaning (hopefully) individual is much more limited in how he can affect your circle of influence than you probably thought. Although limited, his influence is still an important part of the route to recovery.
The doctor has four main options with you once a diagnosis has been made. He can send you to some form of therapy, prescribe medication for pain and/or inflammation, perform surgery or some combination of the 3. Once this decision has been made, the role of the doctor becomes more of an evaluator. He evaluates the impact of the intervention he prescribed and determines to continue, modify, stop or apply one of the other 3 options available. The doctor’s role becomes smaller and smaller after an accurate diagnosis has been made.
Sometimes the doctor’s evaluation and your personal assessment of progress may not match. The case usually being that the doctor feels you have progressed or improved more than you think you have. This difference in opinion brings us to a critical crossroads in your history book. Because if you are not as improved as the doctor thinks you are, or should be, and are still struggling with the pain, then there must be a reason. The possible reasons that run through most people’s minds are that the doctor made the wrong diagnosis. The drugs prescribed weren’t effective or the therapist didn’t “make me well”.
Perhaps it is to your advantage as an individual seeking an improved quality of life, to consider some other possibilities -possibilities outside the contemporary “menu” of options most adhere to. Medications top the list on this contemporary treatment menu, just look at the profit margins for the pharmaceutical companies in this country. If medication is part of your daily regimen for coping with musculoskeletal pain, it doesn’t have to be.
Medications are nothing more than an adjunct to your path to a pain free life. They are not the foundation. And they are certainly not the ultimate answer to your problems. There is not a single medication on this earth that on its own, relieves pain, stops inflammation, fights infections, etc. The only way medications can do their job, is to assist the other systems in the body to do their jobs more effectively.
Am I telling you to flush all of your medication down the toilet right now? No. But I am going to give you hope as to why you should be able to one day. That hope should be inspiration to start formulating a plan to get off your anti-inflammatories and pain killers. Of course I am going to add, “check with your doctor first”. But keep in mind, pain pills and anti-inflammatories are not life and death drugs, as say, blood pressure medication might be. So getting off of these drugs is as much your decision, if not more, as it is your doctor’s.